Natalie* walks down the grime-covered stairwell and through the off-white hallway lined with square speckled tile that makes even the dirtiest of floors appear clean. She passes an eternally propped-open door to the laundry room and various other closed doors, likely to hold mechanical and electrical workings of the building along the way. The smell of detergent, dryer sheets, and fresh laundry stacked on top of dryers and washers by college students, impatient for their turn, fills the air. As Natalie nears the end of the hallway, she passes a sad kitchen and begins to hear her two friends talking. She wonders how long they had been down there before they texted Natalie asking her to join them. At the end of the hallway there is a large, warehouse-like room where colorful couches, tables, and uncomfortable chairs overcrowd the space. She smiles as her friends come into view and takes a seat to the right of Mikayla who sits across from Sarah as they all say hello.
Sarah and Mikayla immediately complain of studying for too long, acknowledging their own insanity in staying down in the basement of Martin Luther Hall until past 1:00 am that night. They beg Natalie to fill them in about her day, her boyfriend Matt, her classes, what she ate for dinner, or anything at all to get their minds off of the psychology topics they had been drilling for the last hour or so. Exams run rampant at this time of year, with only a few weeks left before finals, tension, stress, and workload exceed that of any other time of the semester. Natalie told Sarah and Mikayla about her art project, conjuring up some much-needed distraction. She spread out her blank canvas, soon to be filled with the most important aspects of her hometown and explained her vision for her final project. Quickly losing interest in the art and getting relief from a quick study break, Sarah and Mikayla turn back to their work; deadlines and exams crept closer with each hour chime of the Haas bell tower and there was no time left to mess around.
After working for many hours, to the tune of psychology terms and ideas, the studious trio decides to give up for the night. They pack up their things and lazily climb to their respective rooms upstairs.
Feeling the weight of sleep on her tired eyes, Natalie at last climbed into bed. Just as she does every night, she switches on the fan that sits on the top shelf of her desk so that the air blows directly onto her. Her boyfriend Matt’s XL Manhattanville Baseball sweatshirt and her extra plush blankets piled on top of her keep the breeze from chilling her too much. Once she settles into bed, she avoids the grips of sleep by turning her attention to one last social media comb-through. Natalie eventually ends up mindlessly scrolling through Facebook and reads clickbait articles one after another. She can’t explain why she or any of her fellow peers would do such a thing before bed, but somehow it had become part of her routine.
Usually, she drifts off to sleep not long after the articles tire out her eyes. This night however, was different.
BZZZZZZZ bzzzzzz bzz bzz bzzzzzzz BZZZZZZZZZ
Natalie’s brows furrow upon feeling as if her head is buzzing or vibrating.
BZZZZZZZ bzz BZZZZZZZZZ
As the vibrations get more intense, she notices her hand holding her phone is shaking. No, her whole entire body is shaking — the kind of uncontrollable shaking that happens when someone dares to stay in the swimming pool for ten minutes too long and the cool evening breeze catches their wet bathing suit.
But why? Is this anxiety? Natalie had experienced waves of anxiety that passed quickly, but this was different. She felt like it may never end.
Twenty-five minutes tick by on her phone as she lays there shaking. She tries to go back to Facebook. Snapchat. Instagram. Anything. But, she can’t. Her phone doesn’t even look real. She decided to get up, peeling back her covers. Something was really wrong. She made her way down from her bed and out into the common area on the fourth floor. She noticed an unfamiliar girl there who seemed to be working on a paper at the ungodly hour of 2:00 a.m.. Natalie realizes she had forgotten her glasses and everything around her is blurry. The buzzing in her head grows louder…BZZZZ. She starts to feel as if she is no longer in her trembling body, that she is in a place where she has no control. At last, she looks in the girl’s general direction as her presence is acknowledged and realizes her heart is racing. Her chest tightens even more.
“I– I’m having a really bad panic attack,” Natalie admitted for the first time to this total stranger still shaking. Her mind had gone through a million other possibilities of what could be happening, but she couldn’t get past how it felt like a never-ending tsunami of anxiety. Her body laid horizontally across a plastic, easily cleanable chair. “Oh my gosh, I’m so sorry. Uh… If you need anything just uh… let me know,” the stranger replied. Not knowing what to do, Natalie decided that she needed to call someone for help, someone that wasn’t this total stranger who had better things to do. But who would she call?
According to the Cleveland Clinic, up to 11% of Americans experience a panic attack each year. While panic attacks stem from feelings of fear and anxiety and not from one singular trigger or inciting incident, they often also cause physical symptoms like a racing heart, difficulty breathing, tingling, trembling, and sweating — which leads sufferers, like Natalie, to call 911 thinking they are dying or having a heart attack.
In fact, psychiatric emergencies (including panic attacks) account for 12% of all EMS responses in U.S. and European EMS systems, despite the fact that diagnosing patients is not within the scope of practice of EMTs. This means panic attacks usually result in a trip to an emergency department — possibly a waste of time and money considering that less than 10% of emergency room (ER) visits for panic attacks end up being admitted to the hospital. Worse, only 13% of anxiety-related ER patients saw a mental health specialist.
The care that results from calling 911 and subsequent transport will not help patients long-term and may even harm patients suffering from a panic attack. The use of benzodiazepines — ultimately what results from a trip to the ER — have been shown to have only modest effects on long-term management of anxiety and prevention of returning ER trips. Benzodiazepines, or benzos can also lead to addiction and are a mere bandage of a solution to the deeper problem of uncontrolled stress or anxiety in an individual.
If one’s main source of care for a panic attack or anxiety disorder is a visit to the ER, it will result in expensive and often unnecessary treatment that burdens the healthcare system averaging $42.3 billion for anxiety related disorders alone.
When you call 911, a voice will respond with the all too familiar phrase from dramatized TV and movie renditions of a dispatcher’s job: “911, what is your emergency?” And, in an instant, first responders, like police officers, EMTs and sometimes firemen are off to the races. At any EMS station, the warnings that a call has been placed are loud enough to wake, or rather scare anyone out of the deepest sleep. One-by-one the EMTs adjust their masks and climb aboard the ambulance, gathering the few tidbits of information available to them about what they will soon be walking into.
Even in the busiest of rush hour traffic, the ambulance finds a way through the madness. Of course, the flashing lights and the wailing siren might help. Passerbys pray for the safety and well-being of the patient, trained to do so at the sight or sound of an emergency vehicle. Speeding cars seemingly forget or ignore the law to pull over to make way for the ambulance. Frightened little girls cry at the loud siren while their big brothers giggle with excitement over the action. The little ones don’t quite understand what an ambulance is or what the people who work on them do. Quite honestly, most people have no idea what it’s like unless they’ve caught a ride on one themselves — even then, they probably don’t remember that the inside smells of bleach, or that the chains on the underside of the truck clink the entire way to the destination.
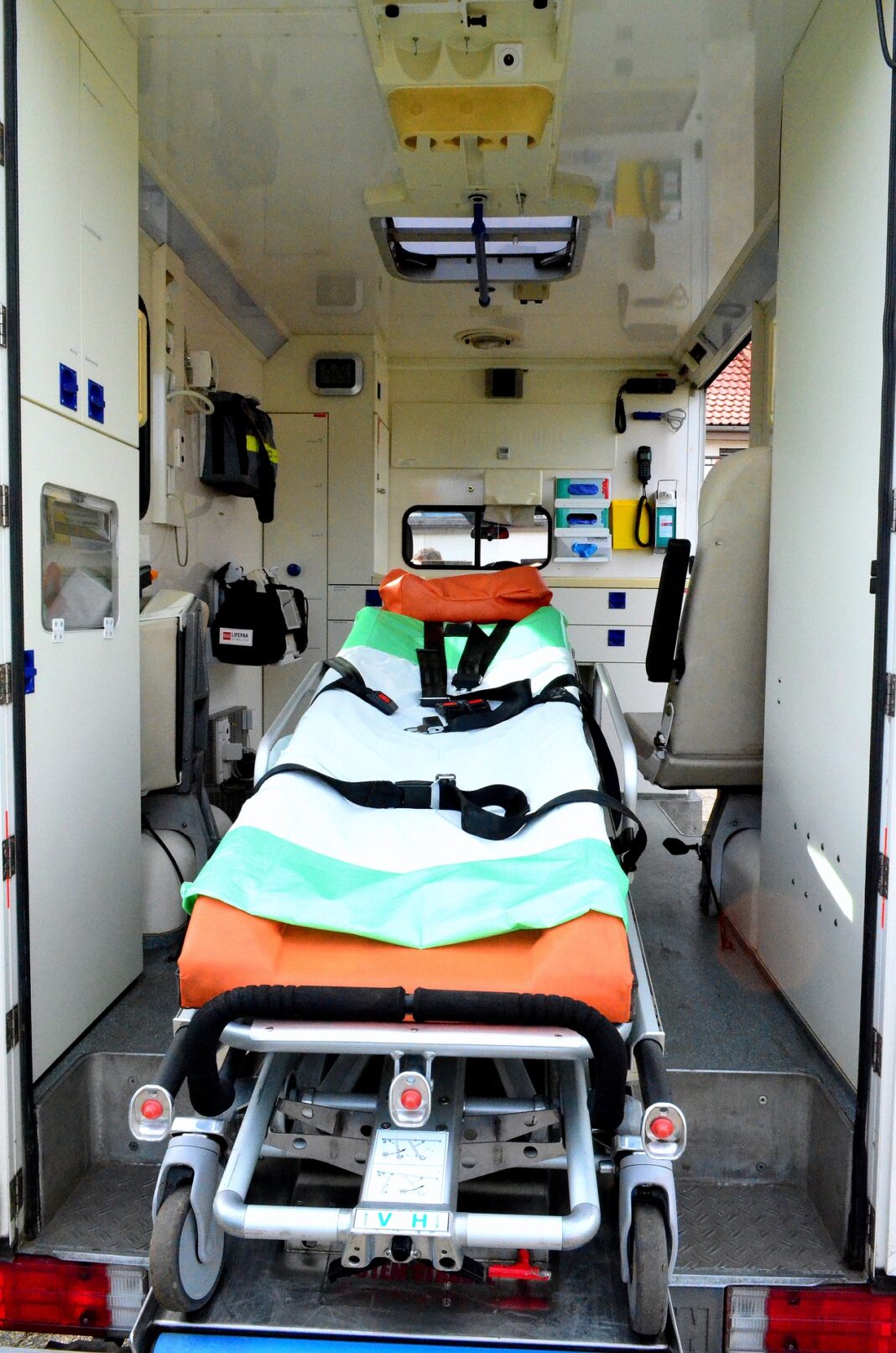
The unforeseen reality is that an ambulance is just like any other car. Four wheels guided by a steering driver bump along highways, byways, freeways, city and residential streets. Each pothole, curb, or small bump in the road jostles the contents inside as if driving over Mount Everest in one go. The medical equipment lines the sides of the truck in clear, numbered cabinets. The hospital-grade spray cleaner streaking each sliding cabinet door obscures the contents inside. Sterile casings crinkle whenever new equipment is opened and the chains clink clink clink.
Fitting into the cabinet array like puzzle pieces are benches where crew members take a seat while working. A blanket warmer sits close to the door to the main driver cabin, where if you’re lucky, a teddy bear lays to comfort little ones that take a ride in the ambulance. Beyond the benches is a sink and above it, a wall covered in a user-friendly control panel. Lights illuminate the crud and dirt in each small crevice on the non-slip floor and spotlight the main attraction of an ambulance: the patient.
Packed full of supplies like splints, tubes, nasal cannulas, gloves, gowns, scissors, tape, oxygen, a stretcher — the list goes on and on and on — the ambulance has something to help most people. But, what about patients like Natalie who are experiencing a mental health crisis? Does it hold something able to help her or would the influx of police officers, EMTs and flashing lights cause her more distress? Would she have felt safe in the glaring attention of so many uniformed people with loud radios and sirens in the distance?
Natalie was experiencing a panic attack, which simply put is an extreme form of sympathetic arousal. What this means is that the fight or flight response is in overdrive and cortisol hormone levels spike. Cortisol is usually referred to as the stress hormone but is more aptly called the “get stuff done hormone,” by Tim Silvestri, Muhlenberg College’s Director of Counseling Services and a licensed psychologist. With a spike in cortisol comes a lot of fleeing or fighting. Even more, it leads to survival. Natalie’s body was in survival mode but had no apparent or clear stressor that would normally elicit this response — she wasn’t standing face to face with a jaguar in her dorm room.
So, if Natalie wasn’t in peril, what caused her panic attack? For some people, the answer lies in one’s stress over time. When someone repeatedly gets knock after knock after knock from various stressors — like failing a test, breaking up with a significant other, losing a job- – there reaches a point where they enter a state of distress where it is difficult to revert back to normal. When only one or few of these events occur like a fender bender or an upcoming bill is due, individuals have coping strategies that help them come down from that stress response. The difference lies in the ineffectiveness of go-to stress relievers such as exercise, spending time with friends, or relaxing to help return the person to a state of well-being. Once they hit this level of distress, it’s really hard to recover.
Eventually, without treatment by a skilled professional such as a therapist or counselor one’s frontal lobe can reduce in volume by one-third. This causes one’s temperament to lack regulation and one’s actions aren’t always decision-based. This unfortunate whirlwind of effects leads to depression and/or panic attacks.
Obviously, Natalie was in some major distress, a state of emotional dysregulation. In that instance, she required skilled care to help herself back to a state of well-being. Physiological changes like increased cortisol lead to a decrease in slow-wave sleep. There are ties between lack of sleep and lack of eating well to fuel one’s body. This lack of fuel leads to resources being rationed for necessary functions in the brain. Heart rate and breathing controlled by the medulla are the top priority while the frontal lobe dives into a state of reduced activity without life-sustaining duties. More specifically, the orbitofrontal cortex and anterior cingulate cortex do not fire at adequate levels and therefore shrink. This is why Natalie woke up suddenly and started shaking uncontrollably.
Natalie’s panic attack lasted far too long without one simple tool: a focusing technique. Our sympathetic and parasympathetic responses are binary systems — the sympathetic nervous system is represented by feelings of anxiety and the parasympathetic by focus. But because they are binary systems, we can either be anxious or focused but not both at the same time. So, the treatment for a panic attack is rather simple, get the person to focus on something. But focus on what? Dogs bark when their humans come home out of delight (parasympathetic arousal), but they also bark when they feel threatened (sympathetic arousal). Yet the barks sound different — dogs changing the pitch of their barks is an example of the vagus nerve. An excited, high-pitched greeting occurs when the dog is happy and excited, while the deep, low pitched snarl accompanies threatened feelings as a warning to others. Humans are the same; in distress, humans respond well to high-pitched sounds. So, the first step in treating a panic attack is to talk in a higher pitch, somewhat like you would to a frightened child.
The second step is more difficult. How do you get someone with a racing heart, abnormal breathing, and in the throes of anxiety to focus? Ask questions. Ask the individual to describe something in the room — how many lights are there? What color clothes are they wearing? Anything to completely distract and focus them on something else so that they can switch off the anxious feeling and switch on the focus. Dr. Silvestri asserts that if what the patient is experiencing is indeed a panic attack, this technique will be successful in a range of 30 seconds to two minutes. Simple. Easy. Effective.
EMTs have various strategies for handling patients in the throes of a panic attack. Nour Yousry said she handles panic attacks by “speaking with a proper tone, asking her questions slower, and not seeming rushed. You want to serve as a social support.” Lindsay Scott says that she “spoke in clear, calm sentences” and she does her best to be “supportive and nonjudgmental.” Katelyn Graver says it’s important to “let these individuals know that we support them and want to help, whether that is through sharing resources, helping them find professionals on campus to talk to, or being there when they are in the most need for someone to listen to them in order to make sure that they are not a harm to themselves or others.” Interestingly, the most common advice given was the specific instruction to “get down to the patient’s level.”
While all of these answers are on the right track, these EMTs struggled to be specific in their responses. Not one of them could describe the how. How does one “serve as social support?” How does one be “supportive and nonjudgmental?” Perhaps this is due to the fact that the EMS curriculum and training disregard mental health and focus almost solely on treating physical symptoms. “The majority of [approaches to panic attack calls] just come from my own personal experiences and what I think would be the best fit for their mission,” explained Nour. The majority of EMS work seems to fall into this category — learning from the more experienced crew members on the job rather than incorporating evidence-based techniques into the curriculum especially with mental health.
Almost no EMT would have suggested using the focusing technique taught by Dr. Silvestri because there is no guideline or competency for caring for mental health in most EMS organizations. This unfortunate lack of regulation around this type of emergency leads to an excess of E.R. visits, some of which may not be necessary. Moreover, continuity of care is an important part of mental health crisis resolution. EMTs are not the ones that can offer care that will solve underlying mental health issues. They are not trained to do so. But they can connect patients with suggestions of available resources. This may alleviate continuous suffering of the individual and can help find solutions to return the individual to a state of well-being instead of masking problems with temporary fixes that leaves the patient in distress.
Why, then, is this not the common practice of EMTs? Would Natalie’s panic attack have ended two hours sooner if only she had called?
“If I could go to a hospital and get injected with some magical drug that would make it all stop, I would do it,” she explained while in crisis. But still, calling 911 never crossed Natalie’s mind. Instead, Natalie went through her list of contacts to find someone who could help her. She immediately crossed her mom off the list. If she called her, knowing her mom, she would drive all the way to Pennsylvania — the four-hour journey for a fearful mother of a struggling child would not be very helpful for either party. She cycled through her other go-to people. After five attempts to reach her boyfriend, she knew that he was asleep and nothing was going to wake him until his alarm the following morning for class. She didn’t want to wake up her roommate, Katie, because her organic chemistry exam was in less than 10 hours that she studied all week for. Besides, Katie and Natalie were not as close as some of her other friends.
Eventually, she settled on her friend Mikayla. She knew that Mikayla was familiar with her battle with anxiety, often confiding in her. But then she remembered Mikayla told her earlier that night that her phone charger broke, forcing her to use a shorter one that doesn’t reach her bed. This left her phone out of reach. Natalie’s thoughts raced as she kept running through her list, hoping for the relief of a familiar voice. Finally, she called Sarah, someone she’s comfortable sharing this vulnerable experience with.
After a few rings the call was declined.
But then, suddenly, a text appeared on her phone.
“Hey what do you want? Maya is asleep, I don’t want to wake her up.”
Through tremors and welling eyes on the verge of tears she manages to text back, “Hey, I need help. I’m having a really bad panic attack. Can I come downstairs and can we sit in the hallway for a little?”
“Yeah, of course.” Sarah replied. “Be right there.”
Natalie made the right call.
*Names were changed due to the sensitivity of medical information divulged by the subject of the narrative.
Photo by Detmold via Pixabay